PubMed Central, CAS, DOAJ, KCI

Articles
- Page Path
- HOME > J Yeungnam Med Sci > Volume 39(3); 2022 > Article
-
Focused Review article
Ultrasound-guided interventions for controlling the thoracic spine and chest wall pain: a narrative review -
Donghwi Park1
 , Min Cheol Chang2
, Min Cheol Chang2
-
Journal of Yeungnam Medical Science 2022;39(3):190-199.
DOI: https://doi.org/10.12701/jyms.2022.00192
Published online: April 26, 2022
1Department of Physical Medicine and Rehabilitation, Ulsan University Hospital, University of Ulsan College of Medicine, Ulsan, Korea
2Department of Physical Medicine and Rehabilitation, Yeungnam University College of Medicine, Daegu, Korea
- Corresponding author: Min Cheol Chang, MD Department of Physical Medicine and Rehabilitation, Yeungnam University College of Medicine, 170 Hyeonchung-ro, Nam-gu, Daegu 42415, Korea Tel: +82-53-620-4682 • Fax: +0504-231-8694 • E-mail: wheel633@gmail.com
Copyright © 2022 Yeungnam University College of Medicine, Yeungnam University Institute of Medical Science
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
- Ultrasound-guided injection is useful for managing thoracic spine and chest wall pain. With ultrasound, pain physicians perform the injection with real-time viewing of major structures, such as the pleura, vasculature, and nerves. Therefore, the ultrasound-guided injection procedure not only prevents procedure-related adverse events but also increases the accuracy of the procedure. Here, ultrasound-guided interventions that could be applied for thoracic spine and chest wall pain were described. We presented ultrasound-guided thoracic facet joint and costotransverse joint injections and thoracic paravertebral, intercostal nerve, erector spinae plane, and pectoralis and serratus plane blocks. The indication, anatomy, Sonoanatomy, and technique for each procedure were also described. We believe that our article is helpful for clinicians to conduct ultrasound-guided injections for controlling thoracic spine and chest wall pain precisely and safely.
- Thoracic spine and chest wall pain is less prevalent than lumbar or cervical area pain, but it has been reported to affect 13% to 15% of the total population [1]. Encountering patients with thoracic spine and chest wall pain in actual pain clinics is not rare in clinical practice. Moreover, persistent thoracic spine and chest wall pain could impair activities of daily living and cause decline in the quality of life [2]. Clinicians generally do not prefer injection to the thoracic structures due to the risk of pneumothorax caused by puncturing a lung with the needle during the procedure. Even with fluoroscopy-guided thoracic procedures, the lungs cannot be viewed directly, meaning any procedure-related risk of pneumothorax is unavoidable [3]. Rather than perform such procedures, clinicians prescribe anti-inflammatory analgesics and physical therapy to patients with thoracic spine and chest wall pain and monitor their progress; however, in several cases, pain is not often controlled sufficiently.
- Ultrasound offers the advantage of being able to perform a procedure with real-time viewing of major structures, such as the pleura, vasculature, and nerves, which cannot be viewed by fluoroscopy [4-7]. Therefore, the ultrasound-guided injection procedure not only prevents procedure-related adverse events but also enables accuracy.
- This study aimed to describe ultrasound-guided interventions that could be applied for patients with thoracic spine and chest wall pain. In this study, the ultrasound image was obtained using an ultrasound machine (RS80A, Samsung Medison Corp., Ltd., Seoul, Korea) with 1 to 7 MHz curved and 3 to 12 and 2 to 9 MHz linear array transducers.
Introduction
- 1. Indication
- The thoracic facet joint injection procedure is indicated for patients with painful conditions due to the involvement of the thoracic facet joints.
- 2. Anatomy
- The thoracic facet is composed of the inferior and superior articular processes. The superior articular processes of the thoracic vertebrae face anteriorly, while the inferior processes face posteriorly [8]. The thoracic facet joints are angled at 60° to the axial plane and 20° to the frontal plane [9]. This allows for rotation and some flexion/extension and lateral flexion. The facet joints are synovial joints, which have a smooth contact surface called articular cartilage [8,9]. Each facet joint is also surrounded by a capsule. An irritated and inflamed facet joint produces mid back pain and thoracic facet-origin pain with reference to the trunk or rib cage [10].
- 3. Sonoanatomy and technique
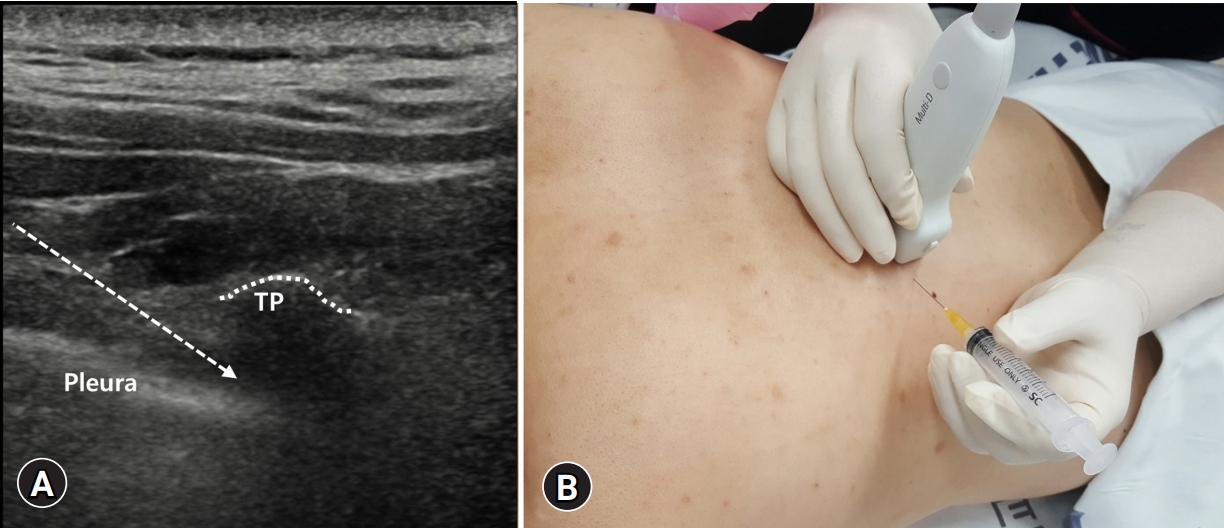
- The facet joint in the thoracic vertebrae has a high coronal plane, which makes it difficult to perform the procedure since the facet joint is not readily visible under fluoroscopy. However, the thoracic facet joint in the coronal plane could be well viewed on ultrasound images, and needle insertion is actually more convenient with ultrasound guidance. The patient is placed in a prone position. After the probe (1–7 MHz curved array transducer) is slightly moved laterally over the lamina, between two hyperechoic lines, that are the inferior and superior articular processes, the thoracic facet joint is visualized in the paramedian sagittal image (Fig. 1A). With the probe in one hand and the syringe in the other, insertion is performed longitudinally toward the proximal region, in-plane below one- or two-finger width below the probe (Fig. 1B).
- To find the level of the posterior joint being targeted by ultrasound, the probe placed longitudinally in the inferior aspect is slowly moved superiorly to locate the 12th rib, which is the first rib visualized. By moving the probe superomedially along the 12th rib, the 12th costotransverse articulation could be seen. By slightly moving inferomedially from this point, the T12 spinous process can be seen past the T12 lamina, which could be used as the starting point. When slightly moving superolaterally from this starting point, the first posterior joint encountered is the T11–T12 facet joint, and the T10–T11 facet joint could be found by moving superiorly. By counting in this manner, the probe could be moved superiorly up to the target joint to perform the procedure. Usually, 1 to 2 mL of local anesthetic is injected per each facet joint.
Thoracic facet joint injection
- 1. Indication
- The costotransverse joint injection procedure is indicated for patients with painful conditions because of the costovertebral joints.
- 2. Anatomy
- The costotransverse joint is the articulation that connects the ribs with the transverse processes [11]. This joint significantly contributes to the stability and movement of the thoracic spine and ribs [11].
- 3. Sonoanatomy and technique
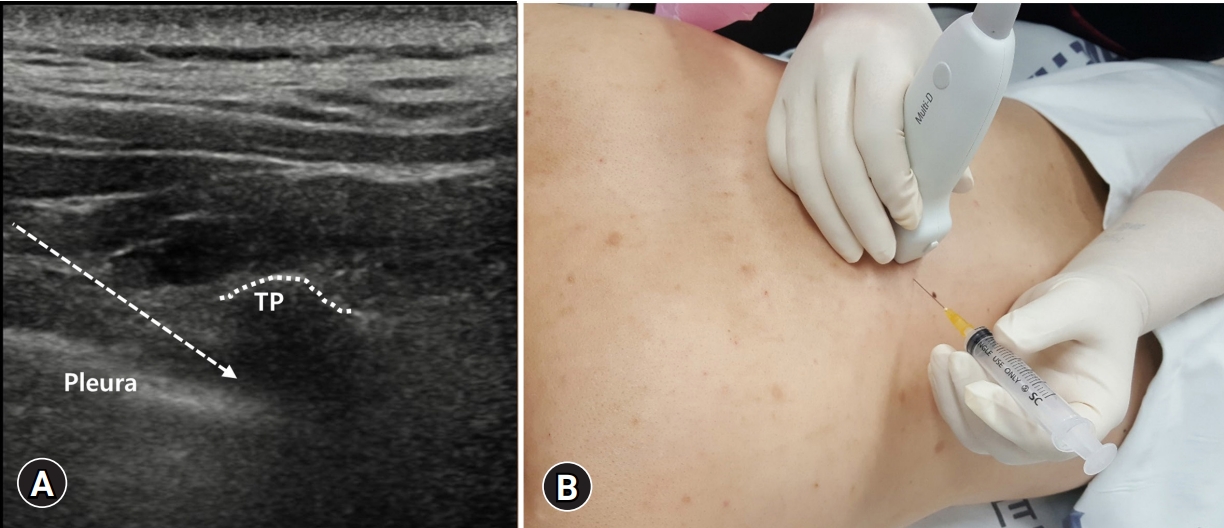
- The patient is placed in the prone position. For the targeted level, the same method previously described in the thoracic facet injection section is used to scan superiorly, starting from the T12 level. Using a 2- to 9-MHz linear array transducer, transverse scan is performed at the targeted thoracic level so that the transverse process, costotransverse joint, rib, and lung appear in the same plane (Fig. 2A). In an in-plane approach, the needle is pointed toward the costotransverse joint in the lateral to medial direction (Fig. 2B). Injection of 1 to 2 mL of local anesthetic is conducted per each facet joint.
Costotransverse joint injection
- 1. Indication
- The procedure can be used in patients with mid back pain, cancer pain on the thoracic spine and chest wall, rib fracture, refractory angina pectoralis, thoracoabdominal neuralgia, or post-thoracotomy pain [12].
- 2. Anatomy
- The thoracic paravertebral space has a triangular shape on axial cross-section, and its borders are as follows: the base is formed by the intervertebral discs, intervertebral foramina, and posterolateral aspect of the vertebral body; the anterolateral border by the parietal pleura; and the posterior border by the superior costotransverse ligament [12]. The thoracic paravertebral space is comprised mostly of fatty tissues, where various nerves, such as the ventral ramus, dorsal ramus, intercostal nerves (ICNs), sympathetic chain, and rami communicantes, pass through [13].
- 3. Sonoanatomy and technique
- The patient is placed in the prone position. The image center is positioned on the lateral side of the transverse process by transverse scan of the targeted thoracic level. The transverse process and ribs are visible from the medial and lateral sides, respectively, as hyperechoic lines. While maintaining the transverse scan, the probe (2–9-MHz linear array transducer) is slid into the intercostal space between the ribs. In the intercostal space, an echogenic line by the pleural interface, instead of the rib, is observed. The intercostal and thoracic paravertebral spaces are visible from the lateral and medial sides, respectively (Fig. 3A). The probe is fixed by the transverse scan in a position with a clear view of the thoracic paravertebral space, and the needle entry site is set to the lateral side of the probe for medial insertion (Fig. 3B). After confirming that the needle tip is inside the thoracic paravertebral space, the injection material is injected into the space (Fig. 3B). The suggested volume is 15 to 20 mL of a long-acting local anesthetic [14].
Thoracic paravertebral block
- 1. Indication
- The ultrasound-guided ICN block procedure is usually necessary for analgesia for multiple rib and sternal fractures, costochondritis, thoracic trauma, chest wall surgery and tumors, and chest tube procedure; postoperative pain control after complete or partial mastectomy, lumpectomy (breast-conserving surgery), or wide excision or breast reconstruction; or the treatment of pain caused by shingles or postherpetic neuralgia [15].
- 2. Anatomy
- The intercostal space is the space between two adjacent thoracic ribs. There are 11 intercostal spaces on each side, and the intercostal muscles, intercostal membranes, ICNs, and intercostal vessels are presented in the intercostal space [15,16]. There are 11 pairs of ICNs (T1–T11), which are the anterior divisions of the thoracic spinal nerves [15,16]. The ICNs course through the intercostal spaces accompanied by the intercostal artery and vein [15,16]. The ICNs provide motor and sensory innervations to the thoracic and abdominal wall and sensory innervation to the peritoneum and parietal pleura [15,16]. Around the posterior axillary line, ICNs are divided into the main and collateral branches [15,16].
- In regard to the intercostal muscles, three layers consist the external, internal, and innermost intercostal muscles [15,16]. The parietal pleura is located under the innermost intercostal muscle [15,16]. From the costal angle onward, a neurovascular bundle, which consists of the main ICNs and vessels, is arranged in the vein, artery, and nerve orientation from superior to inferior [15,16]. Both neurovascular bundles are found between the internal and innermost intercostal muscles. However, the main neurovascular bundle is found near the inferior border of the upper rib of an intercostal space, while the collateral neurovascular bundle is found at the superior border of the lower rib [15,16].
- 3. Sonoanatomy and technique
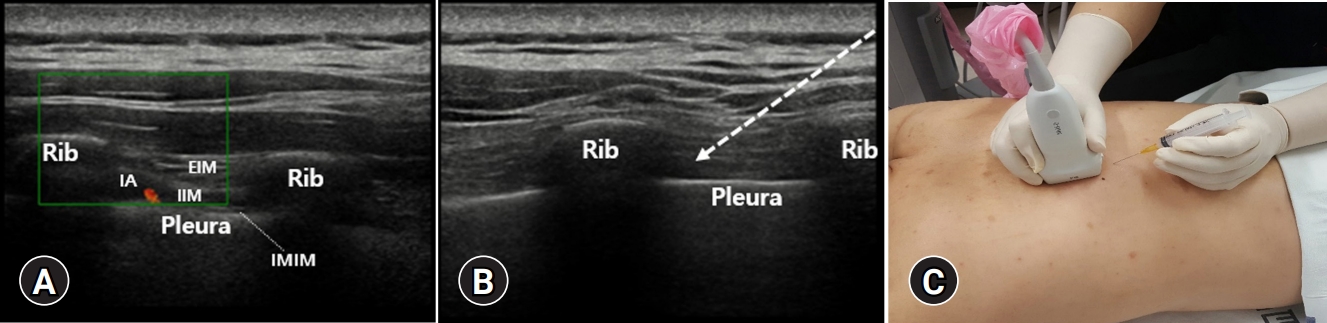
- To perform the effective ICN block by a single injection, an ultrasound-guided ICN block has to be performed before the ICN is divided into the main and collateral branches [15]. Therefore, the ultrasound-guided intercostal block is usually performed at the posterior to the posterior axillary lines. The ICNs in the intercostal space are often not possible to be found by ultrasound examination. However, the vessels within the main neurovascular bundle located in the lower margin of the rib may be visible using the color Doppler (3–12-MHz-linear array transducer) (Fig. 4A). Therefore, it is possible to estimate the location of the ICN by detecting the location of the vessels using a color Doppler.
- The patient can be placed in either sitting, prone, or lateral decubitus position. Using ultrasound, the intercostal space behind the posterior axillary line has to be scanned to find the ICN before dividing it into the main and collateral branches. To identify the level of the intercostal space, start scanning at the inferior angle of the scapula, which corresponds to approximately the 7th intercostal space when the hand is hanging down on the side [13]. After finding the intercostal space, place the probe vertically and advance the needle to the inferior margin of the rib (Fig. 4B, 4C). For ICN block, the injection of 2 to 4 mL of local anesthetic is usually sufficient [16]. However, to improve the effectiveness of ultrasound-guided ICN block, hydrodissection is recommended to distinguish the intercostal muscle layers because these are difficult to distinguish by ultrasound [15].
Intercostal nerve block
- 1. Indication
- The ultrasound-guided erector spinae plane block (ESPB) procedure is usually necessary in patients with thoracic neuropathic pain. Moreover, it is used as a postoperative analgesia method in several surgical procedures from the shoulder to the hip (C7–L4), including laparoscopic/open renal and perirenal procedures and those requiring large dermatomal blockage such as the combination of surgeries (mastectomy, breast prosthesis, and abdominoplasty), urological procedures such as bladder surgeries, radical prostatectomy, gynecological procedures, or orthopedic procedures such as hip and knee surgeries. This block serves the purpose of a paravertebral block without the risk of pleural injury [17,18].
- 2. Anatomy
- The erector spinae is not one muscle but a group of tendons and muscles. It is divided into three columns: iliocostalis (lateral column), longissimus (intermediate column), and spinalis (medial column) muscles [19-21].
- The iliocostalis muscle originates from the iliac crest, sacrum, and erector spinae aponeurosis. It has three different insertions: iliocostalis cervicis (originated from the angle of the 3rd–6th ribs and inserted to the posterior tubercle of the C4–C6 transverse processes), iliocostalis thoracis (originated from the angle of the 7th-12th ribs and inserted to the angles of the 1st-6th ribs, C7 transverse process), and iliocostalis lumborum (originated from the lateral crest of the sacrum, medial end of the iliac crest, and thoracolumbar fascia and inserted to the angles of the 5th-12th ribs, L1–L4 transverse processes) [19-21].
- The longissimus muscle has three parts with different origin and insertion: longissimus thoracis (originated from the sacrum, spinous processes of the lumbar vertebrae, and transverse process of the last thoracic vertebra and inserted to the transverse processes of the lumbar vertebrae, erector spinae aponeurosis, ribs, and costal processes of the thoracic vertebrae), longissimus cervicis (originated from the T1–T6 transverse processes and inserted to the C2–C7 transverse processes), and longissimus capitis (originated from the T1–T3 transverse processes, runs through C3–C7, and inserted to the mastoid process of the temporal bone) [19-21].
- The spinalis muscle has three parts: spinalis thoracis (originated from the T10–L3 spinous processes and inserted to the T2–T8 spinous processes), spinalis cervicis (originated from the T2–C6 spinous process and inserted to the C2–C4 spinous process), and spinalis capitis (originated from the spinous process at the cervical and upper thoracic levels and then inserted to the external occipital protuberance) [19-21].
- 3. Sonoanatomy and technique
- The patient can be placed in either sitting, prone, or lateral decubitus position. Usually, to perform an ESPB at the thoracic level, a high-frequency linear ultrasound transducer probe is used. To identify the spinous process, the probe has to be placed in a transverse orientation.
- Using the previous study as a reference, ESPB can be performed at the T2 vertebral and T5 and T7 spine levels for the sensory blockade of the cervical, thoracic, and lumbar dermatomes, respectively [22].
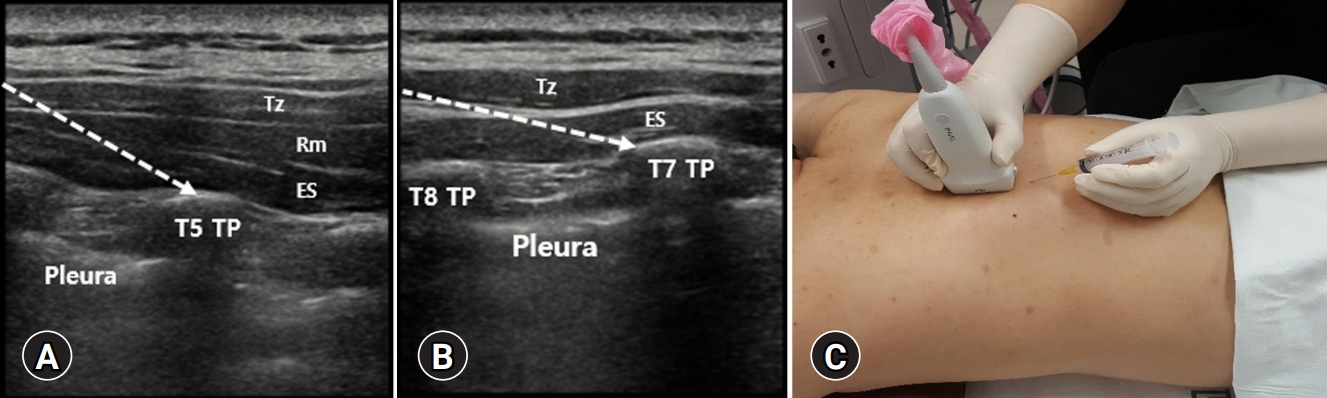
- Using a 2 to 9-MHz linear array transducer, once the level is identified according to sensory blockage level, the probe is moved approximately 3 cm laterally until the transverse process is identified. The transverse process has a square contour compared with the ribs, which has a rounded contour. The probe should be rotated 90° on the transverse process by placing it in a parasagittal plane. At the T5 vertebral level, the following three muscles must be identified as above to the hyperechoic transverse process shadow: trapezius, rhomboid major, and erector spinae (Fig. 5A). At the T7 vertebral level, however, the rhomboid major muscle disappears (Fig. 5B). The needle is usually inserted in the plane (Fig. 5C). Depending on the patient’s position or region to be treated, the procedure can be performed in the craniocaudal or opposite direction. The target of the injection must be in the fascial plane, deeper than the erector spinae muscles at the tip of the transverse process of the thoracic spine (Fig. 5C). To increase the effectiveness, a hydrodissection is recommended.
- In the previous studies, 20 mL of local anesthetics spreads between three and seven levels, averaging the blockage of 4.6 levels. Usually, 20 to 30 mL of local anesthetics is applied in the thoracic spine and chest wall, whereas 30 to 40 mL of local anesthetics is applied in the lumbar areas for the dermatomal coverage of the surgical field [23]. In addition, it is probable that high volume and concentration increase the success rate of ESPB [23].
Erector spinae plane block
- 1. Indication
- The pectoralis (Pecs 1 and Pecs 2) and serratus plane blocks are anterior approach chest wall blocks initially described by Blanco et al. [24] as a novel technique to provide analgesia after breast surgery [25-30]. The Pecs 1 block is targeting the lateral and medial pectoral nerves between the major and minor pectoral muscles. In the Pecs 2 block, the injection of local anesthetic is added under the serratus anterior muscle and into the interfascial space between the pectoralis minor and serratus anterior muscles in addition to the Pecs 1 block. The serratus plane block uses a more lateral and posterior approach to block the interfascial plane superficial or deep to the serratus anterior muscle.
- They can be performed more safely and easily than posterior approach blocks such as thoracic epidural or paravertebral blocks under ultrasound guidance because the anatomical structures concerned are located more superficially and easy to access. Therefore, they could be used as an alternative or emergency option to the posterior approach chest wall blocks when they are not applicable. Although they are originally designed as analgesic options after breast surgery, there are several studies in which they are used for other indications such as rib fracture, thoracotomy, and insertion of a cardiac device [25-30].
- 2. Anatomy
- The pectoral and axillary regions are composed of muscles innervated by the brachial plexus and separated by multiple fascias. The Pecs and serratus plane blocks are targeting these separated interfascial spaces. There are three groups of nerves we should take into account.
- The first group is the lateral and medial pectoral nerves. They arise from the brachial plexus, communicate with each other through the ansa pectoralis, and run between the major and minor pectoral muscles innervating them [31,32]. The Pecs 1 block is aimed at this interfascial space between the major and minor pectoral muscles, expecting to block the pectoral nerves. The lateral pectoral nerve arises from the lateral cord of the brachial plexus, which is supplied from the C5 to C7 nerve roots, runs down in close proximity to the pectoral branch of the thoracoacromial artery, and innervates the pectoralis major muscle [33]. The medial pectoral nerve is a branch of the medial cord of the brachial plexus supplied from the C8 to T1 nerve roots. It runs under the pectoralis minor muscle and then punctures the muscle to enter the interfascial space between the major and minor pectoral muscles [33].
- The second group of nerves is the ICNs, which take charge of the segmental somatic sensory innervation of the chest wall, axilla, and medial aspect of the upper arm. The Pecs 2 and serratus plane blocks are mainly targeting this set of nerves. They give off the lateral cutaneous branches just anterior to the midaxillary line. Thereafter, they run to the sternal border, turn anteriorly, and terminate as the anterior cutaneous branches. The T1 nerve generally has no lateral and anterior cutaneous branches, and most of its fibers join those from the C8 nerve. Some fibers of the T2 and T3 nerves give rise to the intercostobrachial nerve, which innervates the axilla and medial aspect of the upper arm.
- The third and the last group of nerves is the long thoracic and thoracodorsal nerves. The long thoracic nerve arises directly from the C5 to C7 nerve roots, entering the axilla, and resting on and innervating the serratus anterior muscle. The thoracodorsal nerve branches from the posterior cord of the brachial plexus. It accompanies the thoracodorsal artery and innervates the latissimus dorsi muscle.
- 3. Sonoanatomy and technique
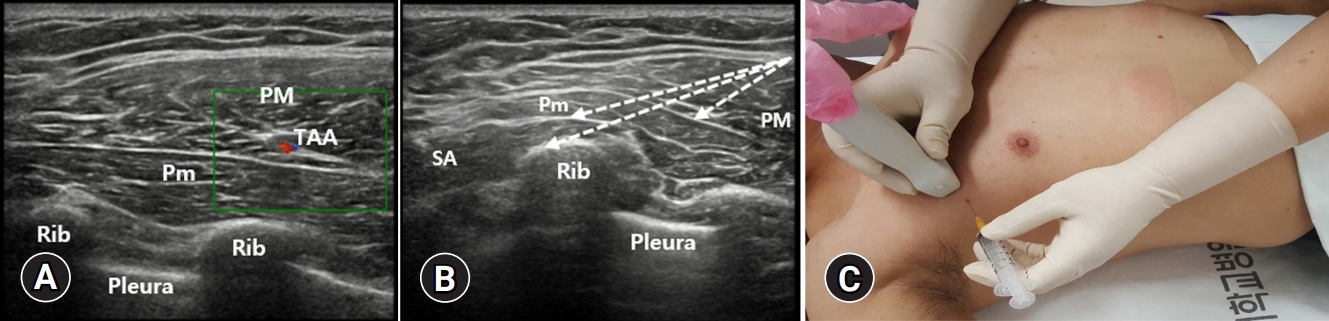
- The goal of the Pecs 1 block is to infiltrate the local anesthetic into the interfascial space between the pectoral muscles to block the lateral and medial pectoral nerves. A high-frequency linear probe (3–12-MHz linear array transducer) is selected because the involved anatomical structures are located superficially. The patient is positioned supine with the arm next to the chest or abducted at 90°. The probe is placed under the lateral third of the clavicle in a sagittal plane where the pectoral muscles and axillary vessels can be visualized. The pectoral branch of the thoracoacromial artery that is in close proximity to the lateral pectoral nerve is seen as a small pulsating structure between the pectoral muscles, and it can be confirmed using the color Doppler ultrasound (Fig. 6A). Rotating the caudal border of the probe slightly laterally, the needle can be introduced from the skin to the interfascial space using the in-plane technique from proximal and medial to distal and lateral in an oblique manner. After confirming the hydrodissection of the two pectoral muscles by the injected local anesthetic, the procedure is completed. The suggested volume is 10 mL of a long-acting local anesthetic [34].
- The Pecs 2 block is an extension of the Pecs 1 block to achieve the blockade of the ICNs, and it includes the Pecs 1 block. From the Pecs 1 block position, the probe is moved more laterally to the anterior axillary line, where the serratus anterior muscle is seen deep and posterior to the pectoralis minor muscle. At the level between the 2nd and 4th ribs, the needle is introduced into the space under the serratus anterior muscle (Fig. 6B). After injecting the anesthetic, the needle is pulled back to the interfascial space between the pectoralis minor and serratus anterior muscles under ultrasound guidance (Fig. 6B, 6C). After injecting the anesthetic, the needle is pulled back to the interfascial space between the pectoral muscles where the Pecs 1 block is performed (Fig. 6B). In that space, the remainder of the anesthetic is deposited. The two targeted interfascial compartments can be blocked with a single skin puncture by this technique, and it is easier to perform the deep block first before the Pecs 1 block. When performing the Pecs 2 block, the first injection of approximately 10 mL of a long-acting local anesthetic is performed into the space under the serratus anterior, and the second injection of 10 mL is performed between the pectoralis minor and serratus anterior muscles (total, 20 mL) [30].
- The serratus plane block is an easier and safer modification of the Pecs blocks, which is expected to block not only the ICNs but also the long thoracic and thoracodorsal nerves. This block is also performed from the anterior approach with an in-plane technique under ultrasound guidance. The patient is in a supine position with their arm abducted. The probe is placed more laterally and posteriorly near the midaxillary to posterior axillary lines. At this location, the latissimus dorsi muscle is seen most superficially and posteriorly (Fig. 7A). The teres major is located superiorly deep to the latissimus dorsi muscle (Fig. 7A). Anteroinferiorly, the serratus anterior muscle is seen deep to the teres major and latissimus dorsi muscles (Fig. 7A). The serratus plane block can be performed superficial or deep to the serratus anterior muscle, but the superficial plane block is safer and more effective (Fig. 7A, 7B) [30]. Compared with the Pecs 2 block, the serratus anterior muscle is more superficially located and easier to identify in this technique; thus, the blockade is easy to be obtained with a low-risk profile. When performing the serratus plane block, approximately 20 mL of a long-acting local anesthetic is administered.
Pectoralis and serratus plane blocks
1) Pecs 1 block
2) Pecs 2 block
3) Serratus plane block
- We believe that our article is helpful for clinicians to conduct ultrasound-guided injections for controlling thoracic spine and chest wall pain precisely and safely.
Conclusion
-
Conflicts of interest
No potential conflicts of interest relevant to this article was reported.
-
Funding
This study was supported by the National Research Foundation of Korea Grant funded by the Korean government (No. NRF2021R 1A2C1013073).
-
Author contributions
Conceptualization, Investigation, Data curation, Formal analysis, Visualization, Validation, Resources, Funding acquisition: all authors; Methodology: DP; Supervision: MCC; Writing-original draft: all authors; Writing-review & editing: all authors.
Notes



- 1. Kim D. Bipolar intra-articular radiofrequency thermocoagulation of the thoracic facet joints: a case series of a new technique. Korean J Pain 2014;27:43–8.ArticlePubMed
- 2. Suzuki N, Ogikubo O, Hansson T. The prognosis for pain, disability, activities of daily living and quality of life after an acute osteoporotic vertebral body fracture: its relation to fracture level, type of fracture and grade of fracture deformation. Eur Spine J 2009;18:77–88.ArticlePubMed
- 3. Lee DG, Ahn SH, Cho YW, Do KH, Kwak SG, Chang MC. Comparison of intra-articular thoracic facet joint steroid injection and thoracic medial branch block for the management of thoracic facet joint pain. Spine (Phila Pa 1976) 2018;43:76–80.ArticlePubMed
- 4. Chang MC, Boudier-Revéret M, Hsiao MY. Ultrasound-guided three-in-one trigger point injection for muscles of the posterior axillary fold. Pain Pract 2020;20:110–1.ArticlePubMed
- 5. Fujii T, Shibata Y, Shinya S, Nishiwaki K. Transverse vs. parasagittal in-plane approaches in ultrasound-guided paravertebral block using a microconvex probe: a randomised controlled trial. Eur J Anaesthesiol 2020;37:752–7.PubMed
- 6. Park D. Ultrasonography of the transverse movement and deformation of the median nerve and its relationships with electrophysiological severity in the early stages of carpal tunnel syndrome. PM R 2017;9:1085–94.ArticlePubMed
- 7. Lee DH, Hong SK, Lee YS, Kim CH, Hwang JM, Lee Z, et al. Is abdominal hollowing exercise using real-time ultrasound imaging feedback helpful for selective strengthening of the transversus abdominis muscle?: a prospective, randomized, parallel-group, comparative study. Medicine (Baltimore) 2018;97:e11369.ArticlePubMedPMC
- 8. Waxenbaum JA, Reddy V, Futterman B. Anatomy, back, thoracic vertebrae. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 [cited 2021 Aug 12]. https://www.ncbi.nlm.nih.gov/books/NBK459153/.
- 9. Jaumard NV, Welch WC, Winkelstein BA. Spinal facet joint biomechanics and mechanotransduction in normal, injury and degenerative conditions. J Biomech Eng 2011;133:071010.ArticlePubMed
- 10. Chang MC. Effect of pulsed radiofrequency treatment on the thoracic medial branch for managing chronic thoracic facet joint pain refractory to medial branch block with local anesthetics. World Neurosurg 2018;111:e644–8.ArticlePubMed
- 11. Lau LS, Littlejohn GO. Costotransverse joint injection description of technique. Australas Radiol 1987;31:47–9.ArticlePubMed
- 12. Ardon AE, Lee J, Franco CD, Riutort KT, Greengrass RA. Paravertebral block: anatomy and relevant safety issues. Korean J Anesthesiol 2020;73:394–400.ArticlePubMedPMC
- 13. Karmakar MK. Thoracic paravertebral block. Anesthesiology 2001;95:771–80.ArticlePubMed
- 14. Hetta DF, Rezk KM. Pectoralis-serratus interfascial plane block vs thoracic paravertebral block for unilateral radical mastectomy with axillary evacuation. J Clin Anesth 2016;34:91–7.ArticlePubMed
- 15. Lopez-Rincon RM, Kumar V. Ultrasound-guided intercostal nerve block. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 [cited 2021 Jul 31]. https://www.ncbi.nlm.nih.gov/books/NBK555900/.
- 16. Glenesk NL, Rahman S, Lopez PP. Anatomy, thorax, intercostal nerves. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 [cited 2021 Jul 26]. https://www.ncbi.nlm.nih.gov/books/NBK538238/.
- 17. Tulgar S, Ahiskalioglu A, De Cassai A, Gurkan Y. Efficacy of bilateral erector spinae plane block in the management of pain: current insights. J Pain Res 2019;12:2597–613.PubMedPMC
- 18. Tulgar S, Kose HC, Selvi O, Senturk O, Thomas DT, Ermis MN, et al. Comparison of ultrasound-guided lumbar erector spinae plane block and transmuscular quadratus lumborum block for postoperative analgesia in hip and proximal femur surgery: a prospective randomized feasibility study. Anesth Essays Res 2018;12:825–31.ArticlePubMedPMC
- 19. Ibbotson WJ, Greenberg R, Brendt P. Erector spinae block for chest trauma in aeromedical prehospital and retrieval medicine. Prehosp Disaster Med 2020;35:454–6.ArticlePubMed
- 20. Elkoundi A, El Koraichi A. Erector spinae plane block dilemma. Reg Anesth Pain Med 2020;45:842–3.ArticlePubMed
- 21. Czuczman M, Shanthanna H, Alolabi B, Moisiuk P, O’Hare T, Khan M, et al. Randomized control trial of ultrasound-guided erector spinae block versus shoulder periarticular anesthetic infiltration for pain control after arthroscopic shoulder surgery: study protocol clinical trial (SPIRIT compliant). Medicine (Baltimore) 2020;99:e19721.ArticlePubMedPMC
- 22. Hong B, Bang S, Chung W, Yoo S, Chung J, Kim S. Multimodal analgesia with multiple intermittent doses of erector spinae plane block through a catheter after total mastectomy: a retrospective observational study. Korean J Pain 2019;32:206–14.ArticlePubMedPMC
- 23. Tulgar S, Selvi O, Senturk O, Serifsoy TE, Thomas DT. Ultrasound-guided erector spinae plane block: indications, complications, and effects on acute and chronic pain based on a single-center experience. Cureus 2019;11:e3815.ArticlePubMedPMC
- 24. Blanco R, Parras T, McDonnell JG, Prats-Galino A. Serratus plane block: a novel ultrasound-guided thoracic wall nerve block. Anaesthesia 2013;68:1107–13.ArticlePubMed
- 25. Kunhabdulla NP, Agarwal A, Gaur A, Gautam SK, Gupta R, Agarwal A. Serratus anterior plane block for multiple rib fractures. Pain Physician 2014;17:E651–3.ArticlePubMed
- 26. Fu P, Weyker PD, Webb CA. Case report of serratus plane catheter for pain management in a patient with multiple rib fractures and an inferior scapular fracture. A A Case Rep 2017;8:132–5.ArticlePubMed
- 27. Kiss G, Castillo M. Non-intubated anesthesia in thoracic surgery-technical issues. Ann Transl Med 2015;3:109.ArticlePubMedPMC
- 28. Kaushal B, Chauhan S, Saini K, Bhoi D, Bisoi AK, Sangdup T, et al. Comparison of the efficacy of ultrasound-guided serratus anterior plane block, pectoral nerves II block, and intercostal nerve block for the management of postoperative thoracotomy pain after pediatric cardiac surgery. J Cardiothorac Vasc Anesth 2019;33:418–25.ArticlePubMed
- 29. Madabushi R, Tewari S, Gautam SK, Agarwal A, Agarwal A. Serratus anterior plane block: a new analgesic technique for post-thoracotomy pain. Pain Physician 2015;18:E421–4.PubMed
- 30. Bashandy GM, Abbas DN. Pectoral nerves I and II blocks in multimodal analgesia for breast cancer surgery: a randomized clinical trial. Reg Anesth Pain Med 2015;40:68–74.ArticlePubMed
- 31. Maldonado KA, Tadi P. Anatomy, thorax, medial pectoral nerves. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 [cited 2021 Sep 3]. https://www.ncbi.nlm.nih.gov/books/NBK556059/.
- 32. Tigga SR, Wadhwa S, Goswami P. Unusual communications of the brachial plexus. Int J Appl Basic Med Res 2016;6:68–70.ArticlePubMedPMC
- 33. Polcaro L, Charlick M, Daly DT. Anatomy, head and neck, brachial plexus. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 [cited 2021 Aug 25]. https://www.ncbi.nlm.nih.gov/books/NBK531473/.
- 34. Fujiwara A, Komasawa N, Minami T. Pectoral nerves (PECS) and intercostal nerve block for cardiac resynchronization therapy device implantation. Springerplus 2014;3:409.ArticlePubMedPMC
References
Figure & Data
References
Citations

- The blind spot and challenges in pain management
Min Cheol Chang
Journal of Yeungnam Medical Science.2022; 39(3): 179. CrossRef

 E-Submission
E-Submission Yeungnam University College of Medicine
Yeungnam University College of Medicine PubReader
PubReader ePub Link
ePub Link Cite
Cite